The Basics
Bevacizumab (brand names- Avastin, Mvasi, Zirabev, Vegzelma, Alymsys) is an FDA-approved treatment for several types of cancer. It is used for cancers in the colon (large intestine), lung, brain, kidney, cervix, ovaries, fallopian tubes, peritoneal layer, and hepatocellular carcinoma. It is also used for a specific type of eye disease, known as age-related macular degeneration.
Bevacizumab is in a class of medications called antiangiogenic agents. They work by stopping the formation of blood vessels that bring oxygen and nutrients to tumours. This may slow the growth and spread of tumours.
let us walk you through the key things you need to know about bevacizumab.
How should I take Bevacizumab (Avastin)?
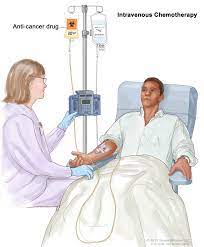
Bevacizumab injection products come as a solution (liquid) to administer slowly into a vein. A doctor or nurse administers bevacizumab injection products in a medical facility.
You should take 90 minutes to receive your first dose of a bevacizumab injection product. If you experience any side effects, tell your doctor immediately.
Do not stop taking abiraterone or prednisone without talking to your doctor. You can help them by tracking your side effects in Ankr.
What are the side effects of bevacizumab or Avastin?
Common side effects
- loss of appetite (34% to 36%)
- heartburn (2%)
- abnormal taste
- diarrhea (21% to 40%)
- weight loss
- sores on the skin or in the mouth
- voice changes
- increased or decreased tears
- stuffy or runny nose
- muscle pain (19%)
- joint pain (28% to 41%)
- trouble sleeping
- headache
- pain in the arms, neck, jaw, stomach, or upper back (12% to 21%)
- extreme tiredness
- weakness
- numbness of an arm or leg
- sore throat
- fever
- chills
- other signs of infection
- swelling of the face, eyes, stomach, hands, feet, ankles, or lower legs
- unexplained weight gain
- stomach pain (8%-10%)
- constipation (4%)
- nausea (53% to 72%)
- vomiting
- shivering
- redness, itching, or scaling of the skin
- pain, tenderness, warmth, redness, or swelling in one leg only
Serious side effects
- nosebleeds or bleeding from your gums (4% to 7%)
- coughing up or vomiting blood or material that looks like coffee grounds (26%)
- unusual bleeding or bruising (17%)
- increased menstrual flow or vaginal bleeding
- pink, red, or dark-brown urine
- red or tarry black bowel movements
- weakness
- difficulty swallowing
- slow or difficult speech
- fainting
- chest pain
- shortness of breath or wheezing (26% to 30%)
- seizures
- dizziness (23%)
- confusion
- change in vision or loss of vision (2%)
- foamy urine
- high blood pressure (24% to 42%)
Bevacizumab injection products may cause other side effects. Call your doctor if you have any unusual problems while receiving this medication.
If you experience a serious side effect, you or your doctor may send a report to the Food and Drug Administration’s (FDA) MedWatch Adverse Event Reporting program online or by phone (1-800-332-1088).
Use the free Ankr platform or Ankr app to track your symptoms.
What special precautions should I follow?
Before receiving bevacizumab or Avastin
- tell your doctor about your allergies
- tell your doctor about other intakes
- tell your doctor about any other disease, symptoms and therapy in the past or now
While you are on bevacizumab or Avastin
- you should know that bevacizumab may cause infertility in women (difficulty becoming pregnant).
- Tell your doctor if you are pregnant or plan to become pregnant. You should use birth control methods after talking to your doctor. Bevacizumab may harm the fetus and increase the risk of pregnancy loss.
- tell your doctor if you are breastfeeding. You should not breastfeed during your treatment with bevacizumab
- tell your doctor if you have recently had surgery or plan to have surgery, including dental surgery. You should not receive a bevacizumab injection if you have recently had surgery.
I forgot a dose. What should I do?
If you miss an appointment to receive a dose of a bevacizumab injection product, call your doctor as soon as possible.
In case of an emergency/overdose
In case of overdose, call the poison control helpline at 1-800-222-1222. Information is also available online at https://www.poisonhelp.org/help. If the victim has collapsed, had a seizure, has trouble breathing, or can’t be awakened, immediately call emergency services at 911.
What special dietary instructions should I follow?
Unless your doctor tells you otherwise, continue your normal diet.
Brand names
- Avastin® (bevacizumab)
- Mvasi® (bevacizumab-awwb)
- Zirabev® (bevacizumab-bvzr)
- Vegzelma®
- Alymsys®
Last Revised – 03/03/2023, FDA updated-10/13/2021, SG
Get 24×7 support for bevacizumab (Avastin)
Don’t go through your cancer journey alone. Use Ankr to:
(1) find the best treatment for your cancer, and
(2) get the advanced warning to cut side effects upto 52%
