Table of Contents
What is Lymphedema?
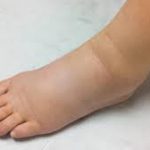
Lymphedema is an abnormal buildup of fluid in soft tissue due to a blockage in the lymphatic system. The lymphatic system helps fight infection by carrying lymph throughout the body. Lymph is a colorless fluid that contains white blood cells.
Lymph travels through the body using a network of thin tubes called vessels. Small glands called lymph nodes filter bacteria and other harmful substances out of this fluid. When the lymph nodes are removed or damaged, lymphatic fluid collects in the surrounding tissues and makes them swell.
How bad is my Lymphedema?
Mild: Trace thickening or faint discoloration of skin, aching in the affected area, and tight skin. Most of the time, mild symptoms can be safely managed at home by following the tips given in the section below.
Moderate: The symptoms are total discoloration of skin, pitting of the skin, leathery skin texture, and papillary (a tumor that looks like long, thin “finger-like” growths) formation. It may limit instrumental activities of daily life (preparing meals, managing money, shopping, doing housework, and using a telephone).
Severe: The skin becomes hard and fattier, swelling, frequent skin infection and difficulty with movement. It can limit self-care activities of daily life (eating, dressing, getting into or out of a bed or chair, taking a bath or shower, and using the toilet).
How to manage mild Lymphedema?
Keep track of your symptoms using Ankr (myAnkr web portal or the Ankr app). It will help you describe the discomfort to your doctor or nurse.
A certified lymphedema therapist (CLT) can develop a treatment plan for you, which may include:
- Manual lymphatic drainage (MLD) involves gentle skin massage. It helps blocked lymphatic fluid drain properly into the bloodstream and may reduce swelling.
- Exercising improves the flow of lymph fluid through the lymphatic system and strengthens muscles.
- Complete decongestive therapy (CDT) or complex decongestive therapy combines skin care, manual lymphatic drainage, exercise, and compression.
- Non-elastic bandages and compression garments (elastic sleeves) helps prevent fluid from refilling and swelling after decongestive therapy. Compression garments must fit properly and should be replaced every 3 to 6 months.
- Lymphedema can increase the risk of infection. Keep the affected area clean, moisturized, and healthy. Apply moisturizer each day to prevent chapped skin.
- Avoid cuts, burns, needle sticks, or other injury to the affected area. Wear a broad-spectrum sunscreen.
- Keeping your affected limb raised helps to reduce swelling and encourage fluid drainage through the lymphatic system.
- Low-level laser treatments (LLLT) provide some relief from lymphedema.
- Antibiotics can treat infection.
If you have trouble swallowing or other issues from lymphedema of the head and neck, you may need physical therapy.
How to manage moderate and severe Lymphedema?
Make an appointment with your doctor if you notice persistent swelling in the arm or leg. If you’ve already been diagnosed with lymphedema, see your doctor if there is a sudden increase in the size of the involved limb.
What causes Lymphedema?
The most common causes of lymphedema in cancer survivors include:
- Cancer and cancer surgery in which lymph nodes were removed
- Radiation therapy or other causes of inflammation or scarring in the lymph nodes and lymph vessels
- Blockage of the lymph nodes and/or lymph vessels by the cancer
- A bacterial or fungal infection or disease involving the lymphatic system.
